The Swinging Pendulum: Managing Your Blood Sugar

If we’ve said it once, we’ve said it a thousand times: maintaining stable blood sugar is a key component to thyroid and adrenal health. Insulin, a hormone generated by the pancreas that helps regulate blood sugar, is a foundational hormone, meaning that if you’re on the blood sugar roller coaster, it will be difficult – if not impossible – to regulate other hormones.
Do you often find yourself in “the pit?” Some call it “hangry?” When you get hungry, do you want to cry or bite someone’s head off? Or both? If so, this post is for you.
[You can find Jill’s newly updated (2022) ebook here: Balance Your Blood Sugar, Balance Your Life]
Even if you don’t experience this havoc (a true emergency state for the body), keeping blood sugar stable has big implications for how you burn fat, how your energy is regulated throughout the day, how you sleep, and your emotional stability. And again, how your thyroid and adrenals function.
And many in the functional medicine community say that stable blood sugar is one of the most important factors in aging well.
When you eat, your body must convert your food into energy. Carbohydrates specifically (vs. fat or protein) are converted into sugar (glucose). How easily and quickly your body makes this conversion, in turn, impacts how quickly, how high, and for how long your blood sugar increases.
The goal is to have a steady, gradual increase, followed by a regulated, slow decline that carries you gently to your next meal. You want to avoid an immediate, short-lived spike: the faster and steeper the climb, the more drastic and harder the fall.
Those crashes can cause headaches, weight gain, binges, intense energy dips, mood swings, sugar cravings, irritability, and emotional overreactions. And for some, panic. “The pit.”
When we ask our clients if they ever experience these emotional and mental responses to hunger, many say, “Oh my gosh, yes. I can get so bitchy.”
Over time, this ping-ponging between spikes and crashes can tax the adrenals, hamper thyroid function, and lead to insulin resistance. And is has significant implications for those with PCOS.
Fortunately, keeping your blood sugar steady and in its “sweet spot” isn’t difficult. The most effective strategies are FOOD-based. Here are some suggestions to help you stay in the zone and these first two points (FOOD-based) will go a long, long way in keeping you out of the pit.
1. For the most part, choose foods relatively low on the glycemic index or with low glycemic loads. Glycemic load and glycemic index measure how quickly a food is converted to usable energy (sugar) in the body. The higher the number, the quicker the rise in blood sugar.
Check out Harvard’s database for GI and GL listings for more than 100 foods. Keep in mind, we’d never recommend many of these high GI/GL foods, like cornflakes or Betty Crocker vanilla cake. Sheesh. Please direct your eyes to the WHOLE FOODS on this list.
This little chart can also help >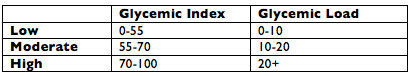
To explain further, foods can have a high glycemic index but a low glycemic load. One example is watermelon, which has a GI of 72 (high), but a GL of 7.2 (low). The GI is based on 5 cups of watermelon (the amount required to reach 50 grams of carbohydrates); the GL is based on an actual serving size of 1 cup.
The GL thus takes into account that watermelon is mostly water, and therefore won’t have much impact on your blood sugar. Other foods that have a high GI but a low GL include carrots, apples, peas, and parsnips.
2. It’s best to eat carbohydrates and proteins with a healthy fat (think nuts and nut butters, fish, olives, avocados, etc.). As described by Gary Scheiner, MS, CDE in his book Think Like a Pancreas, consumption of fat “may slow the digestion of the carbohydrates that were consumed along with the fat, resulting in a slower, more gradual postmeal [blood sugar] rise.”
In fact, we’re fans of Dr. Barry Sears’ 40/30/30 principle. We’re not a big fan of some foods that he advocates (like soy), but the idea that each meal and snack is roughly 40% carbohydrate, 30% fat, and 30% protein is solid advice. It’s about eyeballing your meals – not carrying a gram counter in your pocket.
As for those carbs, make ‘em complex carbs (fruits, veggies, legumes, true whole grains), not simple, rocket fuel carbs that send your blood sugar into the stratosphere (sugar, flour-based foods – you know, processed junk).
3. Engage in 10-15 minutes of physical activity immediately before or after eating. Physical activity diverts blood (and the sugar in it) to fuel the muscles. As recently reported in the New York Times, short bursts of activity before meals lowers blood sugar levels throughout the day. Other research has similarly shown that even a simple 15-minute walk after eating can significantly lower the post-meal blood sugar spike.
Remember, ANY physical activity will be better for blood sugar levels than flopping on the couch or sitting in front of the computer.
4. Try a tablespoon or two of apple cider vinegar (ACV) in a small glass of water before meals, particularly meals that may be higher in carbohydrates. Or use oil and vinegar to dress your salad. Vinegar helps modulate blood sugar swings. (Another tip: a little ACV in water can serve as a great substitute for a sugar-laden glass of wine in the evening.)
5. Add some spice to your life – specifically, cinnamon. Cinnamon is widely reported to help reduce blood sugar levels (as reported here and here). Many of our clients find that incorporating more cinnamon into their diets helps alleviate cravings. Try adding it in your breakfast porridge or smoothie. Add it to coffee. Use it in a spice rub on meat or fish. Drink cinnamon tea mid-morning or afternoon. (You’ll be amazed at what a cup of cinnamon tea will do to slay a sugar craving.)
6. We take a relatively conservative approach to supplements, but chromium or alpha lipoic acid (ALA) can help. Our opinion is that they should be used short-term, in extreme cases, and not as a crutch so that people can continue eating cinnamon rolls for breakfast.
Chromium has been shown to increase the action of insulin.
Alpha lipoic acid has been shown to prevent insulin resistance and can decrease the stress and anxiety associated with low blood sugar. But! The goal is to manage your blood sugar such that you never experience that stress and anxiety. So see, ALA may not be warranted.
7. Eat slowly, chew fully, and breathe deeply. Any stress during meals will cause your body to release stress/adrenal hormones into your bloodstream, which will, in turn, increase your blood glucose levels. This is true any time of day, of course, but we never miss an opportunity to remind folks to keep their stress in check, as there is such an intimate connection between the output of stress hormones/adrenal health and how the pancreas regulates insulin.
Lastly, you can test your blood sugar at home. Find out more here.
Comments
Thank you for the information
Thank you for the information! I just had a micronutrient done and was found to be low in chromium and lipoic acid. I started supplementing chromium (picolinate) about a week ago, but noticed a definite uptick in hair loss. I found others reporting the same side effect online. Have you seen this with any of your patients? Do you know if there is another form of chromium that may not cause shedding?
I am also not sure if it's safe for me to take ALA because I have a mouth full of amalgams.
Thanks so much for any thoughts you may have.
Hmmm, I hadn’t heard of
Hmmm, I hadn’t heard of chromium causing hair loss. I’ve heard people also having good success with GTF (glucose tolerance factor) chromium, so you may want to try that?
Add comment