Low Fat Absorption, Low Hormones

This is the first in a three-part series on the association between gut and hormonal health.
Here’s the second article in the series >
This relationship is incredibly important. It’s why each of my private coaching clients and Gut + Hormone Intensive participants receives both a GI and hormone panel. For a truly comprehensive view of what’s going on, we need both. (Along with some blood markers.)
(As of this writing, the next round of the Gut + Hormone Intensive is opening soon.)
So, you know the drill. The label of “hormone imbalances.” Perimenopause, low estrogen, low progesterone, adrenal issues, hypothyroidism, PCOS…
When it comes to “balancing hormones,” there’s a basic—and not uncommon—issue that’s rarely discussed and it can make the hormone conversation relatively pointless until it’s addressed.
And that is…you can’t build a stable hormonal profile in a system that can’t digest and absorb dietary fat. This post addresses what I feel is one of the single biggest drivers of fat malabsorption.
I’ve been harping on healthy fats for years. In fact, one of my very first articles from 2007 (yes, 19 years ago as of this writing) was called I Hope You Get Fat.
Many think of “cholesterol” when they think of fat. Or more specifically, “I don’t want high cholesterol.” But hey, in 2010 (16 years ago as of this writing), I also wrote an article about the benefits of this critical nutrient called Busting the Cholesterol Myth.
(By the way, hypothyroidism can be a significant contributor to high cholesterol—it can elevate LDL and total cholesterol and impair cholesterol clearance. Don’t let any provider put you on a statin without investigating this possible contributor. And please, don’t even get me started on the dangers of statins.)
I continue to stand by these articles after all this time, even though so many are still hoodwinked by the “high fat = high cholesterol” myth. Indeed, fat and cholesterol are still demonized to a large degree, but not nearly to the extent that they were even a few short years ago.
As they say, you aren’t what you eat, you’re what you absorb. And if you’re not getting enough healthy dietary fats—or absorbing them—your hormones will suffer. How do you know if you’re not absorbing? Keep reading.
Hormones are built from cholesterol
Cholesterol is a building block for estrogen, progesterone, testosterone, DHEA, cortisol, Vitamin D, and bile acids (which you need to digest fat—I’m coming back to this).
I like visuals. And as I recently said in my HRT post, this chart is impressive. It’s also printed on page 329 of our Essential Thyroid Cookbook: Over 100 Nourishing Recipes for Thriving with Hypothyroidism and Hashimoto’s.
Below is another powerful visual regarding a current client.
If fat intake is low and/or digestion is weak, you don’t have the cholesterol to make hormones. And if absorption is compromised, the body can’t reliably use what you’re giving it.
Additionally, you’re not just losing all the benefits of those healthy fats, you’re losing the ability to absorb fat-soluble nutrients like vitamins A, D, E, and K—and essential fatty acids—that help to stabilize the entire endocrine and nervous system. Please read that last sentence again.
It doesn’t mean your body “can’t make hormones,” it’s that it’s trying to run an endocrine system within a digestive system that isn’t optimal.
Fat malabsorption can look like:
- Mood instability
- Anxiety
- Flat mood or low motivation
- Thinning and/or dry hair
- Dry skin (including itchy skin, eczema, scalp issues)
- Dry eyes or “dry everything”
- Irregular cycles
- Worsening PMS with age
- A tough time during pre/menopause (including it being tough for years)
- Brain fog
- Fatigue after meals
- Bloating after meals
- Nutrient deficiencies that don’t respond well to supplementation
- Something weird in the toilet bowl…keep reading
In addition to losing absorption of the nutrients listed above, you can also lose the feeling of true satiation and blood sugar stability.
See why the gut is so important in the hormone conversation?!
Believe me, once digestion and absorption improve, the entire hormonal landscape improves.
Look in the bowl
I ask clients all the time…do you see “egg white” in your stool? Many will say, “Uh, yes, I do.”
(I know, not a pleasant thing to investigate.)
That “egg white” is often the dietary fat you should’ve absorbed. It can also be associated with IBS, general inflammation, and food sensitivities, but I always ask nonetheless. And no, it’s not “diagnostic.”
Fat malabsorption (steatorrhea) doesn’t always show up as “obvious” fatty stools—you may not see mucous in the toilet. It can also look like pale or light-colored stools, stools that float or break apart easily, and oily sheen in the water. (Again, not fun to think about.)
Or it can look like nausea, heaviness, or bloating after fatty meals; feeling “off” after richer foods; or somewhat of an aversion to fat.
An objective way to know: the overlooked bottleneck
The gut panel I provide in my practice measures steatocrit that’s a marker of fat in the stool. High steatocrit is one of the single most prominent indicators of malabsorption, a strong indicator that fat is cruising right on through your system, unassimilated.
To be blunt, all that healthy fat is getting pooped out.
This isn’t a minor issue.
If you’re not digesting fat, you’re not building hormones efficiently. And you’re not stabilizing the nervous system. This is why hormone symptoms can become louder and more disruptive even when you’re doing “all the right things.”
As you can see, “testing hormones” isn’t just about testing hormones.
When steatocrit is high, it’s a pretty clear indicator that fat digestion is compromised and it can create a downstream hormonal problem that “hormone support” simply can’t override.
A common scenario
A woman starts feeling poorly, so she “cleans up” her diet. Maybe lower calorie, lower fat. Does more cardio. Then she starts trying to “fix hormones.”
But if she has poor fat absorption, it can make the situation worse because now she’s not digesting fat well and isn’t eating enough of it to begin with. Not only are hormones made from cholesterol, but the body interprets this as “scarcity” and the entire endocrine system can downshift.
This is why “hormone support” often fails.
You can take all the progesterone, estrogen, DHEA, “hormone balance” supplements, adaptogens, cycle-syncing protocols…the list goes on. But when the digestive system is signaling a fat-handling and bile flow problem, many strategies—including supplements and HRT (hormone replacement therapy)—can seem inconsistent or ineffective because the body cannot reliably absorb, utilize, or clear the compounds involved.
I liken it to bailing water from a leaky boat when what you want to do is plug the leaks. Yes, this is a gross oversimplification and I go much deeper into the alternatives to HRT specifically in this post.
Here’s an example from a current client. This young 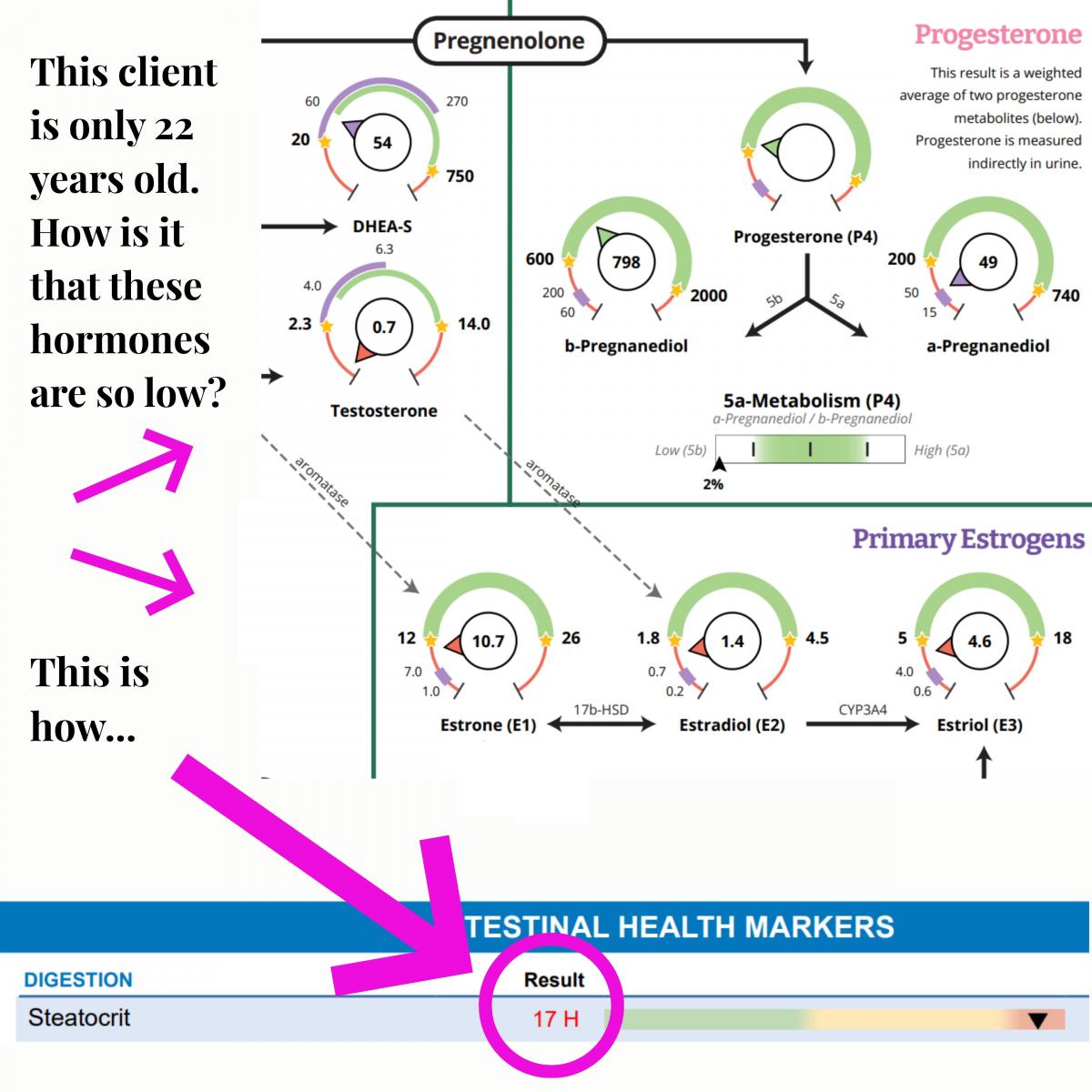
woman is only 22. We received her hormone panel
results prior to her gut panel results and when I saw these hormone levels (or lack thereof), it took me aback. This isn’t normal.
Then we got her stool panel results and everything made perfect sense.
Click on the image for a larger version >
What drives malabsorption?
My non-medical opinion is that the biggest driver of high steatocrit and fat malabsorption is low bile output and/or sluggish bile flow. Bile is required to emulsify fat so it can be absorbed and if it’s
insufficient, fat metabolism is very likely suboptimal.
(And by the way, low bile flow itself can inhibit hormone clearance.)
The liver produces bile that’s either stored in the gallbladder or released into the small intestine to help digest fat.
I’ve harped for years on the role of the liver (“the workhorse”) when it comes to hormone health (we make thyroid hormone conversion largely in the liver, after all) and hormone clearance (especially estrogen).
Poor bile output and/or congested flow can also show up as constipation, nausea with fat intake, bloating after meals, skin issues, feeling worse with supplements, PMS that intensifies with age, and estrogen-type symptoms with “normal labs.”
Now, if sluggish bile is under the hood of high steatocrit, what’s under the hood of sluggish bile? Some common contributors are:
- Long-term stress
- Hypothyroidism
- Low protein intake
- Pancreatic enzyme insufficiency
- Gallbladder weakness (low contraction)
- Gut dysbiosis
- Caloric restriction
You can’t patch a malabsorption problem with HRT
Again, when the gut is indicating a fat-handling and bile flow issue, even HRT can be minimally helpful or even ineffective.
If you have high steatocrit (I can help you test) or you strongly suspect fat digestion issues, the goal is to consider bile flow, gallbladder function (which is strongly linked to liver function, so you’re catching two butterflies with that net), enzyme output, and other possible dysbiosis.
I’m tellin’ you, these have everything to do with your hormones—it’s the terrain that hormones function in.
No, this doesn’t have to be complicated.
Everyone is different and will have different symptoms and contributing factors, but below are some basics. You want to know what you’re dealing with before diving into a protocol. Inside the Gut + Hormone Intensive (or a private coaching program), we assess all of this with the data and personalize an approach.
- Get adequate protein and healthy fat intake—bile flow improves with both. Yes, even if you feel that you have a malabsorption issue, it doesn’t mean you want to decrease or stop eating healthy fats because a low-fat diet often makes the problem worse by reducing the stimulus for bile release.
- Eat bitter foods like arugula, dandelion greens, radicchio, endive, escarole, mustard greens, bitter melon, grapefruit, lemon peel (and other citrus peel), and artichokes.
- Consider digestive bitters. I like Better Bitters by Herb Pharm.
- Consider supports like Lipo-Gen by Metagenics, ox bile, or Lipotropic Complex by Integrative Therapeutics (which contains some ox bile).
- Support your liver—which again, also supports gallbladder function. The liver makes bile. The gallbladder stores and releases it. So anything that improves bile production in the liver indirectly supports gallbladder function.
- Do what you can to get pooping. If stool isn’t moving daily, bile and hormones are more likely to recycle rather than clear.
- Support your adrenals because chronic stress reduces stomach acid, enzyme output, and bile flow and digestive capacity improves when the nervous system isn’t stuck in fight-or-flight.
(For #3 and #4, go here to set up an account and get 15% off retail.)
The specifics—and why different people need different strategies—depend on what’s actually driving the fat malabsorption in the first place. That’s exactly what I do inside the Gut + Hormone Intensive.
Together, we’d:
- Look at the data
- Map your symptom pattern
- Identify your dominant driver(s)
- Address digestion, clearance, and regulation
- Stop the loop so that you have a better hormonal profile
Again, as of this writing, it’s opening soon. Stay tuned by subscribing to my newsletter if you’re not already (scroll up on this page and look to the left—the form is under the image of the cookbook). And stay tuned for the next installments of this three-part gut and hormones mini series!
Comments
I find this very enlightening
I find this very enlightening. Further to all this, how does all this work if I have both Hashimoto's/hypothyroidism as well as my gall bladder removed over 4p years ago. If you could address this scenario that would be helpful. Thank you.
Thank you for this article.
Thank you for this article. So helpful. Something weird that not a lot of the west deals with, but that I am (Oregon resident) is that I have been drinking rain water for the rainy seasons here in the rainier region. So most months of the year, I have not only been getting insufficient minerals from my water supply but also being flushed out by water that is DRAINING my electrolytes. Based on immense and intense research (again thank you, this article has helped a lot) I have come to realize I 100% have been effected by the lack of minerals in my water and have fat malabsorption due to this cause. It has also taken a major toll on my hormones! Redirecting now to trace minerals and adding that to every cup I drink!
Add comment